If you or someone you love has diabetes and has noticed a sore on the foot that just refuses to heal, a toe that has turned dark, or a wound that keeps getting worse no matter how much care you give it, please do not ignore it. These could be signs of diabetic ulcers, and early attention can truly be the difference between saving and losing a limb.
This guide has been written to help you understand what diabetic ulcers are, why they happen, how to spot them early, and, most importantly, what you can do about them. Dr. Himanshu Verma, a leading vascular and endovascular surgeon based at Fortis Memorial Research Centre, Gurugram, sees patients every week who come in with non-healing wounds, and he wants you to have this knowledge before things get worse.
What Are Diabetic Ulcers?
Diabetic ulcers are open sores or wounds that most commonly develop on the feet and lower legs of people living with diabetes. They are classified as chronic wounds because they tend to be stubborn and do not heal the way a normal cut or scrape would. In fact, even a small blister, a minor cut, or a slight skin breakdown can turn into a serious diabetic foot ulcer if left unattended.
The reason diabetic ulcers are so dangerous is that diabetes affects the body in multiple ways at once. It damages nerves, reduces blood flow, and weakens the immune system. This means a person with diabetes may not even feel a wound forming on their foot due to a condition called peripheral neuropathy. By the time they notice it, the wound is already deep and possibly infected.
Why Does My Wound Not Heal? Understanding the Real Cause

This is one of the most common questions Dr. Himanshu Verma hears from patients. They say, 'Doctor, I have been applying ointment for weeks, but this wound just does not close.' The answer lies in understanding what diabetes actually does to your body.
- High Blood Sugar Slows Everything Down: Prolonged hyperglycemia quietly damages blood vessels and nerves over the years. It thickens your blood, weakens immune cells, dries out skin, and slows new cell formation all of which make wound healing a prolonged, difficult process.
- You Can't Feel the Damage: Diabetic nerve damage (peripheral neuropathy) means you may not feel pain, pressure, or heat in your feet. A small stone in your shoe becomes a blister, a blister becomes a wound, and because you feel nothing, you keep walking on it, making it worse every day. This is how most diabetic foot ulcers begin.
- Your Blood Isn't Reaching the Wound: Diabetes also narrows the arteries supplying your feet and legs (Peripheral Arterial Disease). Without adequate blood flow, tissues are starved of oxygen and nutrients. Wounds can't heal, infection spreads, and in severe cases, tissue begins to die from necrosis.
Early Signs of Diabetic Ulcers You Should Never Ignore
The earlier you catch a diabetic ulcer, the better the outcome. Dr. Himanshu Verma always tells his patients that catching a wound in Stage 1 is worlds apart from treating it in Stage 4. Here are the signs you should watch out for closely, especially if you have diabetes and live in areas like Gurgaon, Delhi NCR, Noida, or Haryana, where access to vascular care may require some planning.
Physical Signs on the Foot or Leg
- A sore, cut, or blister that has not healed in 2 weeks or more
- Redness, warmth, or swelling around a wound area
- Pus or any discharge coming from a wound (a clear sign of infection management need)
- A foul or unusual smell coming from the wound or shoe
- A darkening or blackening of the skin, especially the toes (possible sign of gangrene)
- Skin that looks cracked, dry, or peeling on the soles or heels
- A corn or callus that has broken open underneath
Symptoms You Might Feel
- Burning, tingling, or complete numbness in the feet (peripheral neuropathy symptoms)
- Pain that worsens at night or when lying down
- Cramping in the calves when walking (a sign of poor circulation)
- Cold feet even in warm weather
- Feet that look pale, bluish, or discolored
The Connection Between Diabetic Ulcers and Blocked Arteries

Many patients focus on keeping the wound clean and controlling blood sugar; both are necessary, but often not enough. The underlying cause of most chronic diabetic wounds is blocked arteries, known as Peripheral Arterial Disease or PAD.
PAD occurs when fatty deposits narrow the arteries supplying blood to the legs and feet. Without adequate blood flow, no dressing, no antibiotic, and no ointment will allow a wound to heal. The tissue is simply not receiving the oxygen and nutrients it needs to recover.
This is frequently missed. Patients spend weeks on wound care while the real problem, a blocked artery, goes undiagnosed and untreated.
Warning Signs of PAD
- Leg pain or cramping when walking that eases with rest
- Cold or numb feet
- Weak or absent pulse in the foot
- Shiny, hairless skin on the legs
- Slow-growing toenails
- A wound that does not respond to any standard treatment
How Are Diabetic Ulcers Treated?
There is no single approach. Diabetic Ulcers Treatment depends on the wound's severity, infection status, and blood supply.
1. Blood Sugar Control: The foundation of everything. No wound heals when blood sugar remains uncontrolled.
2. Wound Debridement: Dead and infected tissue is removed to create a clean base for healing to begin.
3. Wound Dressing: The right dressing depends on wound depth, type, and discharge. This is a clinical decision made case by case.
4. Infection Management: pus, spreading redness, or fever requires immediate antibiotics. If the bone is affected, surgical intervention may be necessary.
5. Offloading: Walking on a wound stops it from healing. Pressure is removed using special footwear, casts, or mobility aids.
6. Restoring Blood Flow: If arteries are blocked, angioplasty, stenting, or bypass surgery is performed. Without circulation, nothing else works.
7. Negative Pressure Wound Therapy: For deep or complex wounds, gentle suction draws out fluid, reduces swelling, and stimulates tissue growth.
How to Prevent Diabetic Ulcers
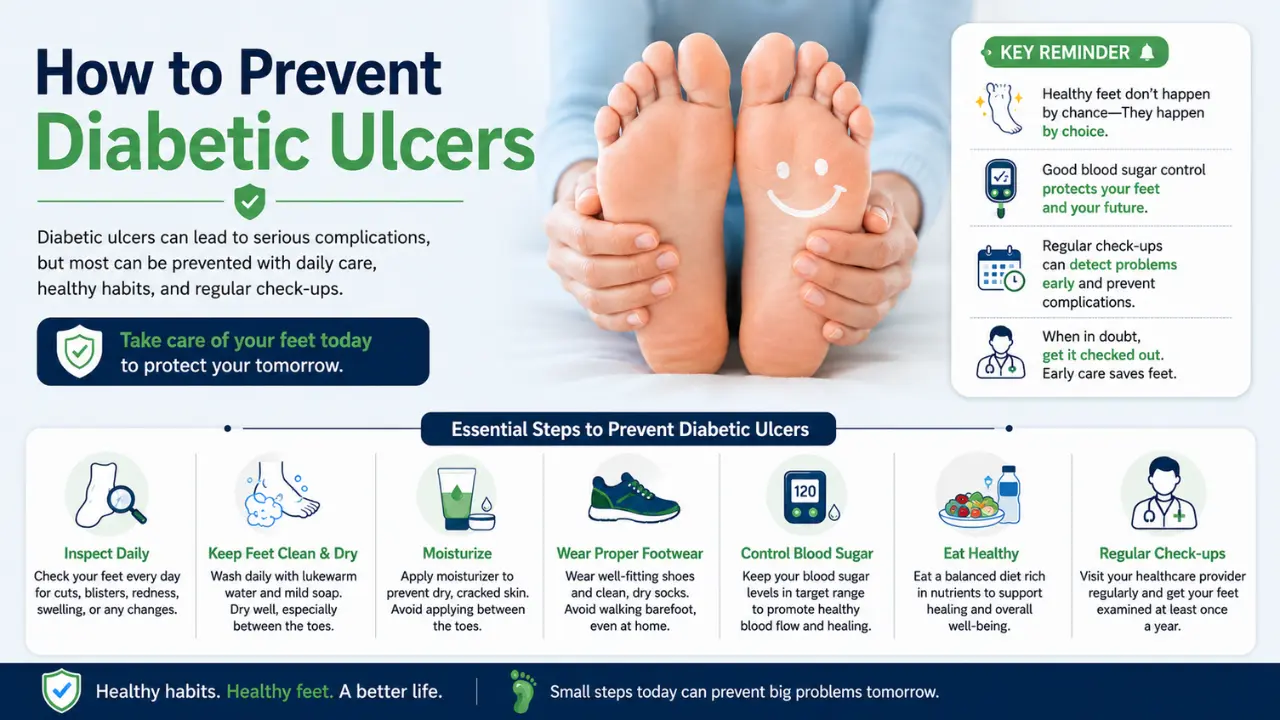
Most diabetic foot problems are preventable. These habits, followed consistently, make a significant difference.
- Daily Foot Care: Wash feet daily with lukewarm water and dry thoroughly, especially between the toes. Moisturise the soles and heels, but never between the toes. Inspect your feet every day for cuts, blisters, redness, or swelling. Use a mirror if needed. Never walk barefoot, even at home.
- Footwear: Wear properly fitting shoes and check inside them before putting them on. Avoid tight socks or elastic that restricts circulation. If recommended, use diabetic footwear prescribed by a specialist.
- Medical and Lifestyle Habits: Control your blood sugar. This is the single most important step. Get your HbA1c tested regularly. Have your feet examined at every doctor visit. Do not smoke; it directly worsens circulation and accelerates vascular disease. Stay physically active with low-impact exercise as advised by your doctor.
About Dr. Himanshu Verma, Vascular Surgeon, Gurugram
Dr. Himanshu Verma is a vascular and endovascular surgeon at Fortis Memorial Research Centre, Gurugram, specialising in conditions that affect blood vessels, including Peripheral Arterial Disease, non-healing diabetic ulcers, and limb-threatening ischemia.
Patients travel from across Gurgaon, Delhi NCR, Noida, and Haryana for his care. His approach is straightforward: every option to restore blood flow and save the limb is explored before surgery is considered.
Take the First Step Toward Healing Your Wound
Consult with Dr. Himanshu Verma, an experienced vascular and endovascular specialist at Fortis Memorial Research Centre, who focuses on advanced, limb-saving treatments for complex vascular conditions.
Call Now: 88268 33598
Email: varenyamvascular@gmail.com
Visit Clinic: Fortis Memorial Research Centre, Opposite HUDA City Centre, Sector 44, Gurugram, Haryana 122003
Don’t delay care. With the right treatment at the right time, most diabetic wounds can heal, and complications can be avoided. Book your consultation today and take the first step toward recovery. You can also explore other services, including vascular screenings, preventive vascular check-ups, minimally invasive procedures, second opinions for vascular conditions, and personalised long-term care plans designed to protect your limb and overall health.
Conclusion: Your Wound Has Hope. Act Early.
Diabetic ulcers are serious, but they are also manageable when caught early and treated correctly. Whether you have a small sore that is not healing, a foot that feels numb, or a wound that has turned dark, please do not wait. The longer you delay, the more difficult treatment becomes and the greater the risk of infection, gangrene, and eventually amputation.
Dr. Himanshu Verma has dedicated his career to helping patients like you save their limbs, restore their circulation, and get back to living a normal life. With the right combination of blood sugar control, wound care, vascular treatment, and patient education, most diabetic ulcers can be healed without major surgery.
If you are in Gurgaon, Delhi NCR, Noida, or anywhere in Haryana, you have access to world-class vascular care. Reach out today. Your wound has hope. Your limb has hope.
