Vascular Specialist · Gurgaon
Pelvic Venous Disorders Treatment in Gurgaon
Expert care for Pelvic Congestion Syndrome and related vein conditions - personalized treatment by Dr. Himanshu.
Women
Most Commonly Affected
PCS
Most Common Vein Disorder
Minimally Invasive
Preferred Approach
Same Day
Discharge in Most Cases
Understanding Pelvic Venous Disorders
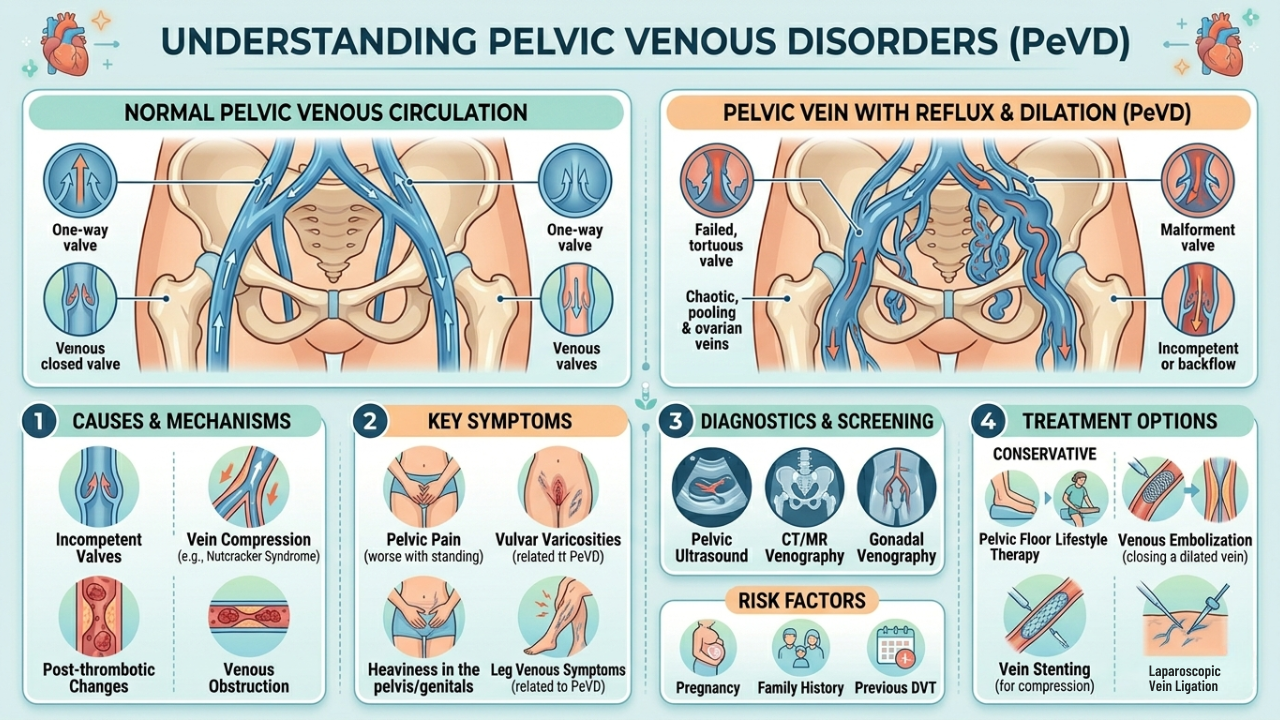
Pelvic venous disorders are conditions where the veins inside the pelvis stop working properly - they become enlarged, twisted, or unable to drain blood efficiently back toward the heart. The most common form is Pelvic Congestion Syndrome (PCS), a condition that causes persistent, often unexplained pelvic pain, particularly in women of childbearing age.
Think of it like varicose veins but inside the pelvis rather than on the legs. Because these veins are internal, the condition is frequently missed or misattributed to gynaecological problems, IBS, or musculoskeletal issues. Many patients wait years for a correct diagnosis. Dr. Himanshu Verma is trained to identify these vascular patterns early through targeted imaging and treat them effectively without major surgery.
Key Facts
What to Look For
Symptoms: What Pelvic Venous Disorders Feel Like
Pelvic venous disorders often cause a dull, aching discomfort in the lower abdomen or pelvic area that many patients describe as a "dragging" feeling. What makes PCS particularly difficult to spot is that symptoms tend to worsen in predictable situations such as prolonged standing, sitting, or after sex and improve when lying down.
Common symptoms include:
If you recognise several of these symptoms particularly if they've persisted for more than three to six months - a structured vascular assessment is the recommended next step. These symptoms are frequently misattributed to other conditions, so a specialist's evaluation is important.
Getting Diagnosed
How Do I Know If I Have Pelvic Venous Disorders?
Because pelvic venous disorders are internal and their symptoms overlap with many other conditions, an accurate diagnosis requires specialised imaging not just a routine examination. Dr. Verma follows a structured, step-by-step diagnostic protocol to confirm PCS and rule out other causes before recommending any treatment.
Medical History & Physical Exam
Identify patterns of pelvic pain through a comprehensive clinical review.
Ultrasound
Check for vein dilation and blood flow issues using non-invasive imaging.
CT or MRI Scans
Obtain detailed views of pelvic veins to assess the extent of the condition.
Venography
Map abnormal vein patterns and confirm Pelvic Congestion Syndrome (PCS).
Treatment Pathways
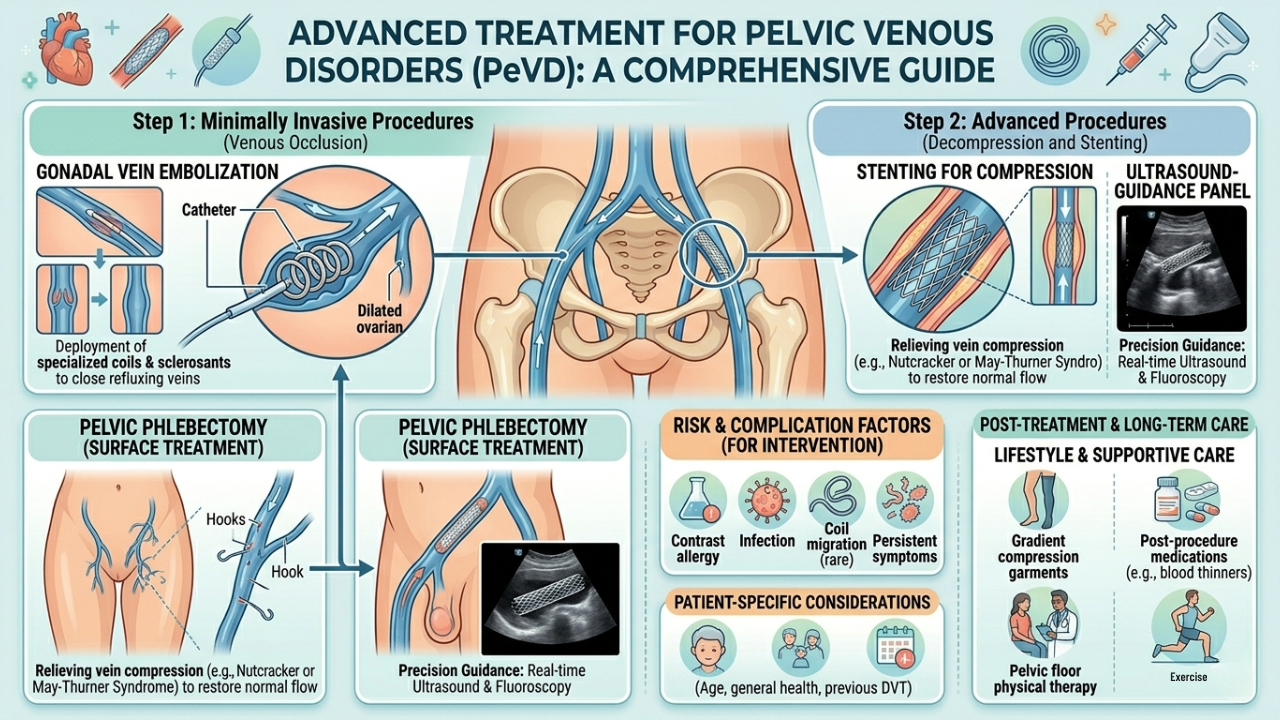
How Are Pelvic Venous Disorders Treated?
Treatment for pelvic venous disorders is tailored to the severity of the condition and the patient's overall health. Dr. Verma evaluates each case individually before recommending a pathway.
Lifestyle & Supportive Measures
First-line ManagementIn early or mild cases, conservative steps can significantly reduce discomfort. These include regular low-impact exercise, avoiding prolonged standing or sitting, wearing compression garments, and using prescribed pain-relief medication where appropriate. While these measures won't resolve the underlying vein problem, they help manage day-to-day symptoms while a formal treatment plan is being organised.
Pelvic Vein Embolization
Minimally Invasive (Gold Standard)Embolization is the preferred treatment for Pelvic Congestion Syndrome and most pelvic venous disorders. It is a catheter-based, image-guided procedure performed under local anaesthesia — no open surgery, no general anaesthesia, and no large incision. A thin tube is guided through a small entry point, typically at the wrist or groin, to reach and seal the malfunctioning pelvic veins. The entire procedure usually takes one to two hours, and most patients go home on the same day.
Clinical evidence shows embolization achieves significant symptom relief in the vast majority of PCS patients, with a low rate of recurrence.
Surgical Intervention
Rare CasesSurgery is seldom required for pelvic venous disorders today. It may be considered in highly complex anatomical situations where minimally invasive options are not feasible. Dr. Verma will discuss this option only where it is genuinely indicated, and all alternatives will be explored first.
Every treatment plan is discussed in full with the patient before any procedure begins. You will always understand your options, the expected outcomes, and any possible risks.
What Causes Pelvic Venous Disorders?
Pelvic venous disorders develop when the valves inside the pelvic veins weaken and stop working efficiently. Healthy vein valves open to allow blood to flow toward the heart and close to prevent it from flowing back. When these valves fail, blood pools in the pelvic veins, causing them to become engorged and painful — similar to varicose veins in the legs.
Several factors can contribute to this valve weakening:
Pregnancy
The most significant risk factor. Increased blood volume and hormonal changes during pregnancy place significant stress on pelvic vein walls. Women who have had multiple pregnancies are particularly at risk.
Hormonal Influence
Oestrogen relaxes vein walls and reduces their tone, which is why PCS is far more common in women and often improves after menopause.
Genetic Predisposition
A family history of varicose veins or vascular conditions may increase susceptibility.
Prolonged Standing or Sitting
Occupations involving long periods in one position can increase pressure in the pelvic venous system over time.
Anatomical Factors
Certain anatomical variants, such as a retroverted uterus or narrowing at the left renal vein (nutcracker phenomenon), can contribute to pelvic vein congestion.
Understanding your specific risk profile helps Dr. Verma determine not only how to treat the condition, but also how to reduce the likelihood of recurrence.
Take the First Step Toward a Clear Diagnosis
If chronic pelvic pain has been affecting your daily life, you do not have to keep guessing. A structured vascular evaluation with Dr. Himanshu Verma at Fortis Memorial Research Centre, Gurugram, can provide a clear diagnosis and — where appropriate — a minimally invasive treatment option that does not require an overnight hospital stay.
Why Patients Choose Dr. Himanshu Verma for Pelvic Vein Treatment
When dealing with a condition as misunderstood as Pelvic Congestion Syndrome, the specialist you choose matters enormously. Dr. Himanshu Verma is a trained Vascular & Endovascular Surgeon with specialist expertise in venous and endovascular conditions, practising at Fortis Memorial Research Centre — one of Gurugram’s leading tertiary care hospitals.
Specialist Vascular Training
Dr. Verma’s clinical background is specifically in vascular and endovascular surgery. Pelvic vein embolization requires precision imaging interpretation and advanced catheter-based skills unique to vascular specialists.
Minimally Invasive, No Hospital Admission in Most Cases
Procedures are performed under local anaesthesia, typically as day-care treatments with faster recovery and minimal disruption to daily life.
Imaging-Guided Accuracy
Every procedure is guided by real-time imaging to ensure precision targeting of malfunctioning veins while protecting surrounding structures.
Fortis Memorial Research Centre
Procedures are performed in a NABH-accredited tertiary care hospital with advanced catheterisation laboratories and complete emergency backup.
Patient-Centred Care
Dr. Verma takes time to explain the diagnosis, treatment options, and expected outcomes. Patients are never rushed into decisions.
Common Questions
FAQs
Diagnosis typically begins with a detailed clinical history and a pelvic ultrasound to assess blood flow patterns and vein diameter. If Pelvic Congestion Syndrome (PCS) is suspected, a CT or MRI scan may be recommended for a more detailed assessment of the pelvic venous anatomy. In some cases, a venogram — where contrast dye is injected and X-ray images are taken — is used to map abnormal vein flow precisely. Dr. Himanshu Verma will explain which tests are appropriate for your specific situation.
The most common cause is weakening of the valves inside the pelvic veins, which allows blood to pool rather than drain efficiently. Pregnancy, hormonal influences (particularly oestrogen), genetic predisposition, and certain anatomical variants can all contribute. Women with multiple pregnancies are particularly susceptible.
Most patients experience minimal discomfort during the procedure, which is performed under local anaesthesia. You may feel mild pressure or warmth at the catheter entry site, but the procedure itself is not typically painful. Mild pelvic cramping in the day or two after treatment is common and is usually well managed with standard pain relief.
Embolization has a high long-term success rate. However, in a small percentage of cases, symptoms may recur if additional veins become affected over time. Dr. Himanshu Verma will discuss your individual risk profile and what follow-up monitoring is recommended after treatment.
While genetic and hormonal factors cannot be changed, maintaining a healthy weight, staying active, and avoiding prolonged periods of standing or sitting can help reduce pressure on the pelvic venous system. Women with a family history of vein disorders may benefit from earlier specialist assessment after pregnancies.
Yes — chronic pelvic pain is the defining feature of Pelvic Congestion Syndrome. The pain typically ranges from a dull ache to a sharp, dragging discomfort and tends to worsen with prolonged standing, physical exertion, sexual activity, and toward the end of the day. Symptoms often improve when lying down.